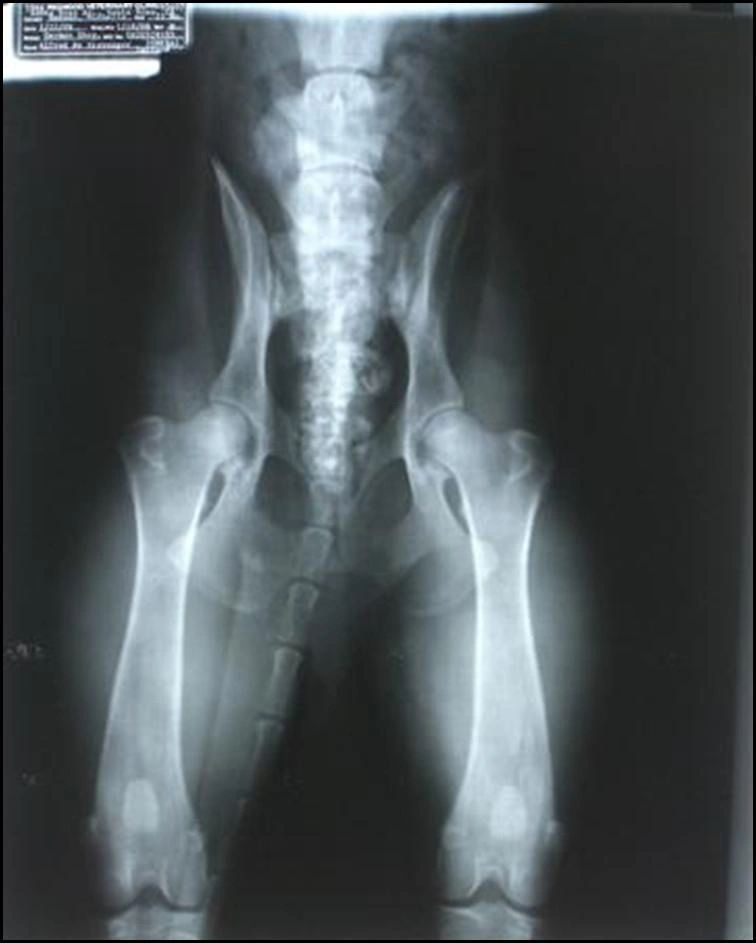
The normal value is still debated, however, there is sufficient agreement that an angle greater than 50° is abnormal and more than 55° is more specific for impingement ( Figure 15 b). 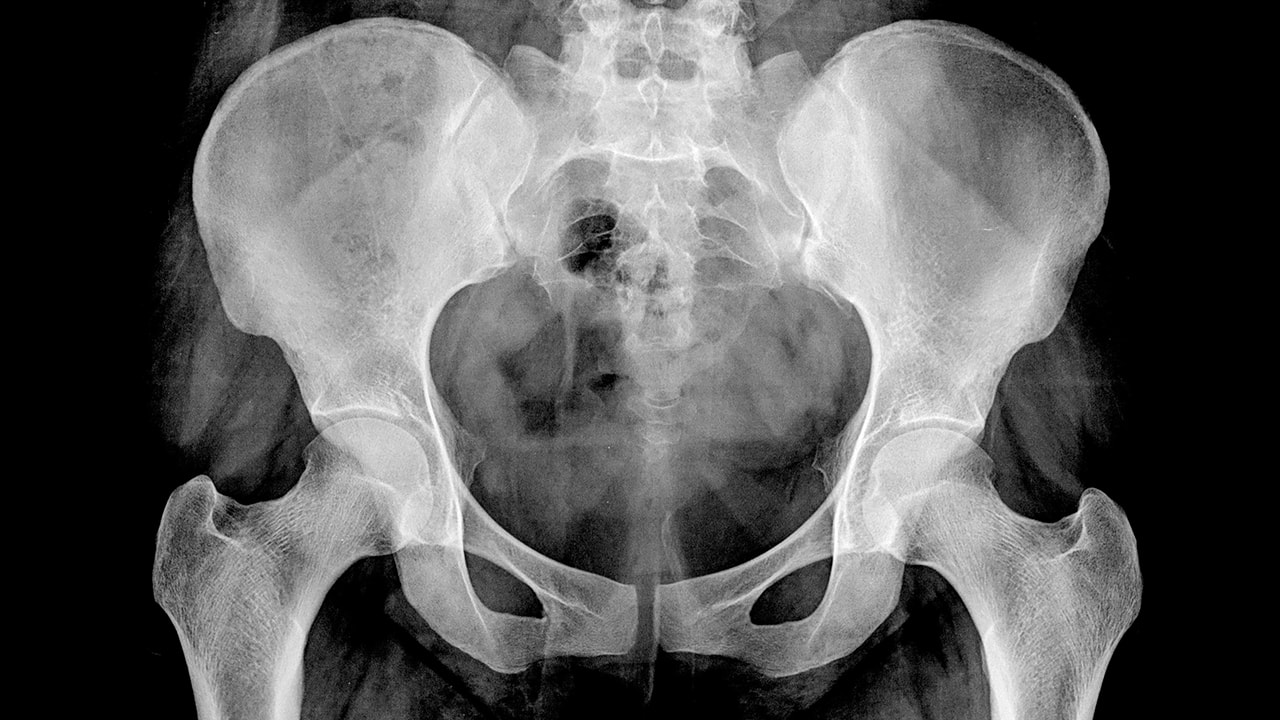
It is defined as the angle between the femoral neck axis and a line connecting the center of the femoral head with the point where the sphericity of the head-neck contour ends. It is a measurement of the femoral head sphericity and evaluates femoral dysplasia 5, 12, 14, 15. The degree of deformity can be calculated by measuring the alpha angle in the cross table projection or in the 45° Dunn projection, although the measurement in the MR axial oblique projection is more reliable. Loss of the anterior femoral offset a) cross-table view, femoral offset (dashed line), bony prominence or bump (arrow) b) Hip MRI axial oblique PD FS. If the diagnosis is FAI, the AP Pelvic view should be taken with lumbar lordosis correction to make the signs and measures of the acetabulum reliable 6 ( Figure 2). The first variable to consider in Pelvic X-ray is quality control, related to symmetry, tilt and rotation ( Figure 1). Pelvis X-ray determines if the hip is normal, borderline or dysplastic, if there are signs of CAM, PINCER impingement or a combination of both, signs of degenerative or inflammatory arthropathy, avascular necrosis, calcifications, tumors, etc. For joint pathology or avascular necrosis: Lowenstein (frog leg lateral) view, etc. To assess anterior acetabular coverage: false profile. For example, if Femoracetabular Impingement (FAI) is suspected: true axial or cross-table, 45° Dunn or 90° Dunn 1, 5. 
The standard study includes Anteroposterior Pelvic view (AP Pelvic view) to evaluate the acetabulum and joint space, which we recommend in standing position because it add information about pelvic slope and acetabular version.ĭepending on the clinical suspicion, some additional localized views of the hip can be used. There are numerous X-ray views to asses non-traumatic hip in adults 1. This article submits to the ethical standards of the journal 4. It is useful for joint anatomy, bone lesions hidden to X-ray and fractures. Computed tomography (CT), which use ionizing radiation, has greater spatial and contrast resolution than X-ray. To assess cartilage in MRI, in addition to the morphological information, dGEMRIC T1 and T2 mapping have been used, which provide information about its composition of water and glycosamino glycans (GAG). 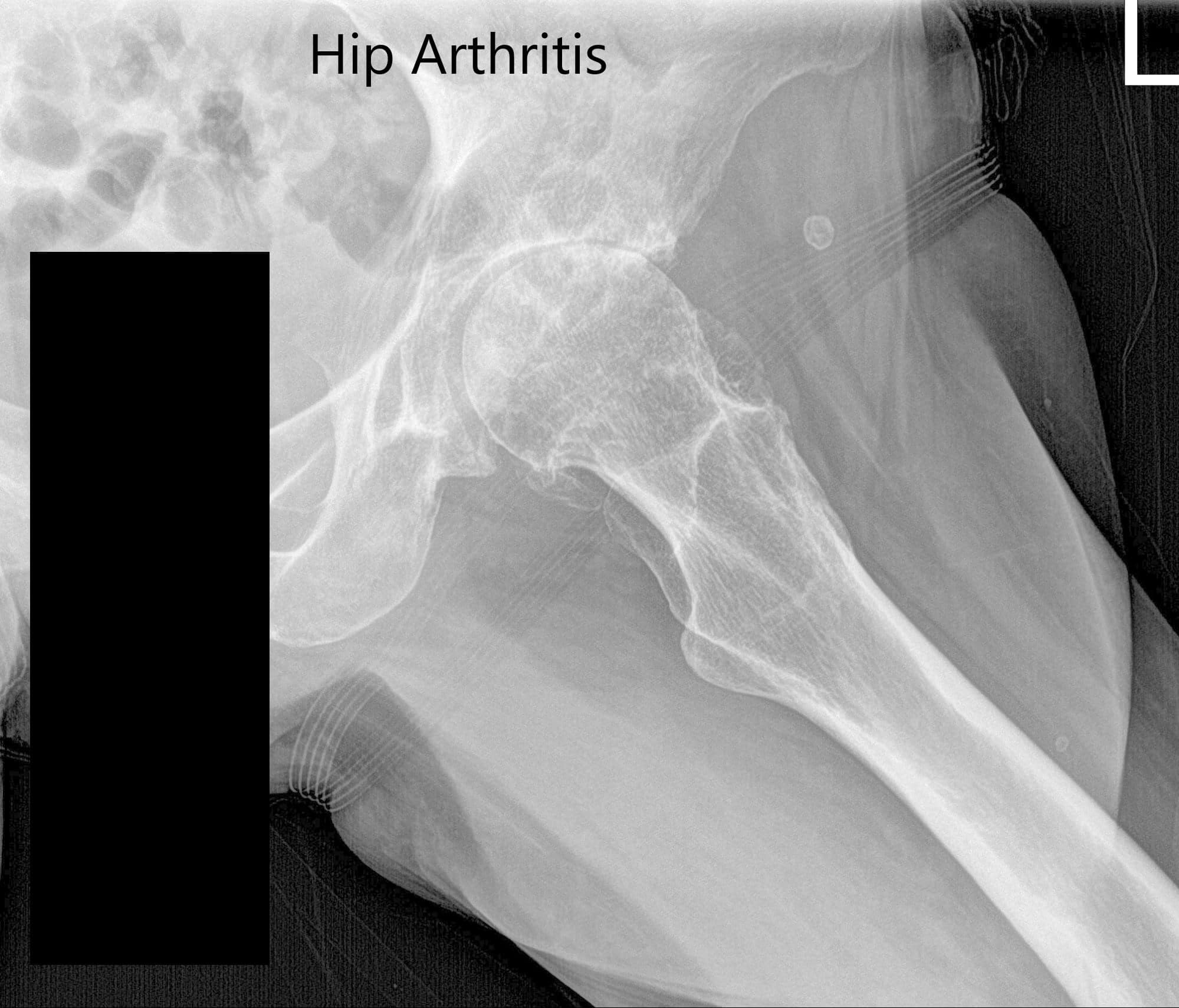
It also can be used to inject a local anesthetic, for example, and perform the “Lidocaine Test”, with clinical diagnostic value. MRI with intraarticular contrast (MR Arthrography) has better performance than conventional MRI for the evaluation of intraarticular pathology, especially of labrum and cartilage. It can also be used as a guide for diagnostic and/or therapeutic procedures. Ultrasound (US) also has a role in the evaluation of peri-articular soft tissues and detection of joint effusion or synovial thickening, allowing dynamic assessment of the joint. The method of choice to assess the bone marrow, acetabular labrum, cartilage and peri-articular soft tissue, is magnetic resonance imaging (MRI). X-ray is the basic tool for the study of the hip 1, 2, 3.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
